“Ulcer” is a scary word for anyone. For diabetics, it’s even scarier.
Those with insufficient blood flow or unchecked blood sugar can experience severe complications from untreated foot ulcers, more so than other individuals.
Let’s look at what puts those with diabetes at higher risk for infection and how you can prevent and treat this concerning foot problem.
What is a Foot Ulcer?
In their simplest form, foot ulcers are open sores or wounds that won’t heal.
There are three types of foot ulcers:
- Venous ulcers, which are often seen in those with leg swelling or vein-related conditions
- Arterial or ischemic ulcers, which affect those with poor circulation
- Neurotropic or “diabetic foot” ulcers, commonly seen on the bottom of the feet of those with diabetes
For the sake of this article, we are going to focus on the diabetic foot ulcers exclusively, although foot ulcers do affect a wide variety of others, including those with foot deformities like bunions or hammertoes, people who wear ill-fitting shoes and more.
Why Are Diabetics More Prone to Developing Foot Ulcers?
Approximately 15% of those with diabetes suffer from foot ulcers, according to Advancing Foot & Ankle Medicine and Surgery (APMA). To make matters worse, 6% of those patients will require hospitalization due to an infection or other complication.
It begs the question, “What puts diabetics at higher risk of getting foot ulcers?”
Elevated blood glucose levels over time can cause nerve damage to the extremities, or a condition called neuropathy.
This nerve damage can make it difficult for diabetics to feel pain in their legs, ankles and feet. Wearing ill-fitting shoes can cause rubbing that produces a wound, walking barefoot can cause a lesion or tight footwear can cause circulation issues. Without the ability to sense pain, these issues often go unnoticed and worsen with time.
This is especially true for older patients, who may lose the ability to reach and care for their feet and neglect to maintain hygiene and routine care.
In addition, elevations in blood glucose can reduce the body’s ability to fight off a potential infection as well as slow healing time. Because of this, diabetics typically have more trouble resisting and recovering from foot ulcer-related issues.
Diabetic Foot Ulcer Symptoms
While ulcers can form in many areas, those with diabetes often suffer from wounds on the bottom/soles of their feet, as this is where the skin is subject to the most pressure from body weight.
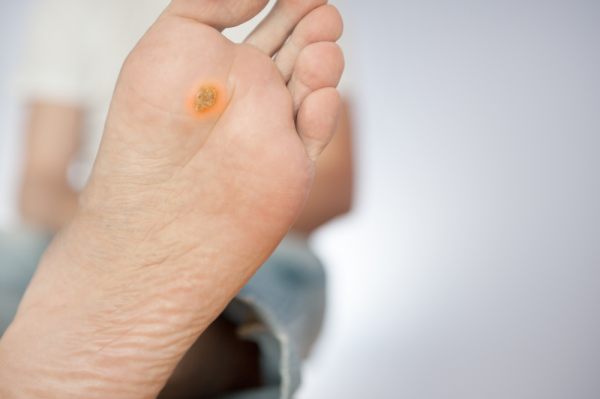
Because neuropathy is common and diabetics often don’t feel pain around the ulcer, sensitivity is often not a symptom.
Instead, here are a few things to look out for:
- Drainage from pussing or oozing
- Redness or swelling around the wound
- A foul-smell, from discharge
- Callused or thickened skin around the sore
- Fevering or chills
Many of these symptoms indicate infection, and if you experience any of these signs, seek treatment immediately.
Diabetic Foot Ulcer Treatment
Diabetics, in particular, are at greater risk of developing infections and take longer to heal, so timely and consistent wound care is incredibly important.
To put it into perspective, approximately 14-24% of diabetics with an ulcer need to get their foot amputated, according to APMA.
Prevent drastic measures by following these foot ulcer treatment recommendations:
- Keep the ulcer covered, clean and moist. Hydrogen peroxide or some sanitation solutions can actually dry out the would and make it worse, so use a mild soap with water to sterilize or a specialized topical cream/ointment for ulcers. Keep the wound dressed to prevent infection or further irritation.
- Off-load your foot. Off-loading simply means keeping weight and pressure off of the sore. This means you must rest and stay off your feet for long periods of time while the foot ulcer heals. A podiatrist may recommend special footwear or accessories such as padded socks to cushion the sore, a brace or even a wheelchair or crutches until the ulcer is gone.
- Carefully remove any dead skin or tissue around the wound. Sanitize your cutting tools and gently clip any “debridement,” which may prevent the sore from properly healing.
- If infected, take proper antibiotics. Infection can be extremely dangerous, so take whatever your doctor prescribes, consistently.
The Diabetic Foot Care You Need
Diabetics can experience a wide range of foot related issues, and it’s critical that they follow these important preventative measures.
If you or someone you love is experiencing a foot ulcer— don’t wait. Infection can progress quickly and in severe cases, lead to amputation.
Our team prides ourselves on our ability to get patients in for same-day appointments for emergencies. Make a quick appointment or give us a call at 239.936.5400, right away.
Categorized in: Blog